Insomnia: Causes, Symptoms, and Evidence-Based Treatments
Learn what insomnia is, its causes, symptoms, and evidence-based treatments. Understand how sleep problems affect mental health and how to improve sleep.
SLEEP
Dr Mahendra Singh
3/10/20264 min read


Sleep problems are common, especially during stressful periods. However, when difficulty falling asleep or staying asleep becomes frequent and begins to affect daytime functioning, it may indicate insomnia.
Insomnia is one of the most common sleep disorders. Studies suggest that up to one-third of adults report symptoms of insomnia, while a smaller proportion develop persistent sleep difficulties associated with daytime impairment.
Although insomnia may begin during periods of stress, illness, or life changes, it can persist even after the original trigger has resolved.
Understanding the causes of insomnia can help identify effective ways to improve sleep.
What Is Insomnia?
Insomnia is a sleep disorder characterized by difficulty:
falling asleep
staying asleep during the night
waking earlier than intended
obtaining restorative sleep
Importantly, insomnia occurs despite having enough time and opportunity to sleep and is usually accompanied by daytime symptoms such as fatigue, irritability, or difficulty concentrating.
For many people, insomnia occurs several nights per week and persists for weeks or months.
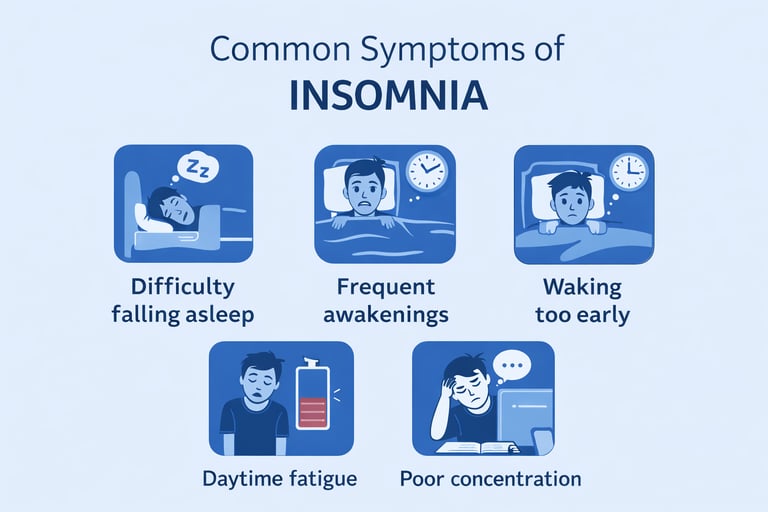
Common Symptoms of Insomnia
People experiencing insomnia may notice:
Difficulty falling asleep at night
Frequent awakenings during the night
Waking too early and being unable to return to sleep
Feeling unrefreshed after sleep
Daytime fatigue or sleepiness
Difficulty concentrating or remembering information
Irritability or reduced emotional resilience
In clinical practice, these symptoms often lead people to seek help when they begin interfering with daily functioning.
Types of Insomnia
Sleep specialists often classify insomnia according to how long it lasts.
Short-Term Insomnia
Short-term insomnia typically lasts a few days to several weeks and is often linked to identifiable stressors such as illness, travel, or emotional distress.
Chronic Insomnia
Chronic insomnia is diagnosed when sleep problems occur at least three times per week for three months or longer and are associated with daytime impairment.
Without treatment, chronic insomnia may persist for years in some individuals.
Why Insomnia Happens?
Insomnia rarely has a single cause. In many cases, it develops through a combination of psychological, behavioural, and biological factors.
A commonly used framework is the 3-P model of insomnia, which describes three types of contributing factors.
Predisposing Factors
Some people may be naturally more vulnerable to insomnia due to factors such as:
genetic predisposition
personality traits such as high worry or emotional sensitivity
female sex
increasing age
Precipitating Factors
These factors trigger the initial sleep disturbance. Examples include:
stressful life events
illness or pain
emotional distress
shift work or irregular sleep schedules
Perpetuating Factors
Even after the original trigger resolves, certain habits can maintain insomnia. These include:
irregular sleep schedules
excessive time spent awake in bed
daytime napping
worry about not sleeping
These behaviours can unintentionally reinforce sleep difficulties over time.
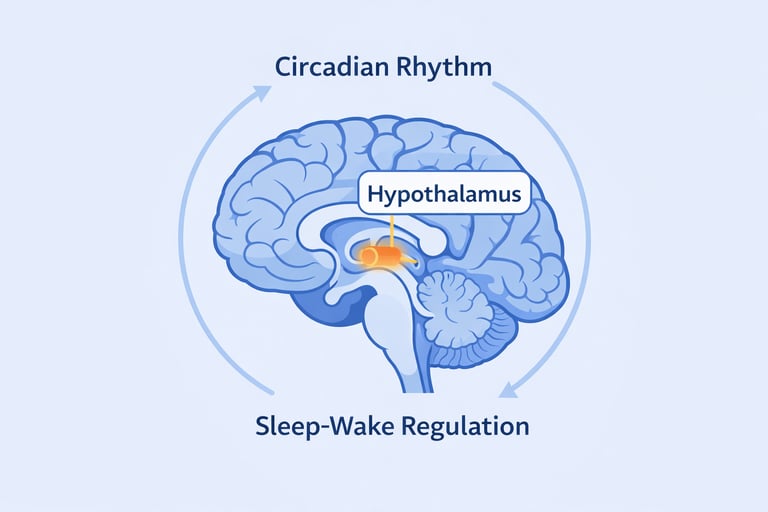
How Insomnia Affects the Brain?
Sleep and wakefulness are regulated by complex networks in the brain involving several neurotransmitters and circadian mechanisms.
Key systems include:
GABA, which promotes sleep
Orexin, which promotes wakefulness
Dopamine and norepinephrine, which support alertness
Serotonin, which helps regulate sleep and mood
Research suggests that many individuals with chronic insomnia experience a state of physiological hyperarousal, meaning the brain remains excessively alert even during the night.
This heightened arousal can make it difficult for the brain to transition into sleep.
Insomnia and Mental Health
Sleep and mental health are closely connected.
Approximately 40% of people with insomnia also have a psychiatric condition, most commonly anxiety or depression.
In many cases, the relationship works in both directions:
mental health conditions can disrupt sleep
persistent insomnia can increase vulnerability to anxiety or depression
Addressing sleep problems often improves overall emotional wellbeing.
Potential Consequences of Chronic Insomnia
Persistent sleep deprivation can affect several areas of functioning.
Common consequences include:
reduced concentration and memory
irritability and emotional reactivity
reduced productivity at work or school
increased risk of accidents
Research suggests that individuals with insomnia may be two to four times more likely to experience accidents compared with good sleepers.
Over time, chronic sleep disturbance may also contribute to broader health problems.
Treatment Options for Insomnia
Effective treatment usually involves behavioural strategies and, in some cases, medication.
Cognitive Behavioural Therapy for Insomnia (CBT-I)
CBT-I is widely considered the first-line treatment for chronic insomnia.
It focuses on identifying and modifying behaviours and thoughts that interfere with sleep.
Common techniques include:
stimulus control (reassociating the bed with sleep)
sleep scheduling and sleep restriction
relaxation techniques
cognitive restructuring of sleep-related worries
CBT-I has been shown to produce sustained improvements in sleep quality.
Improving Sleep Habits (Sleep Hygiene)
Sleep hygiene refers to daily habits that support healthy sleep.
Helpful strategies include:
maintaining a consistent sleep schedule
limiting screen exposure before bedtime
avoiding caffeine late in the day
creating a comfortable and quiet sleep environment
While sleep hygiene alone may not resolve chronic insomnia, it provides an important foundation for healthy sleep.
Medication
In some cases, medications may be prescribed to provide short-term relief from severe sleep disturbance.
Common medications include:
benzodiazepines
non-benzodiazepine hypnotics
melatonin receptor agonists
orexin receptor antagonists
Medication should generally be used under medical supervision and alongside behavioural strategies.


When to Seek Professional Help
Occasional sleep difficulties are common. However, professional evaluation may be helpful if:
sleep problems persist for several weeks or longer
daytime functioning is significantly affected
there are symptoms of anxiety or depression
sleep medications are being used frequently without medical guidance
Early evaluation can help identify underlying causes and guide appropriate treatment.
Insomnia Self-Assessment
If you are unsure whether your sleep difficulties may indicate insomnia, you may consider completing a brief screening questionnaire.
Reviewed by Dr. Mahendra Singh Uikey
Consultant Psychiatrist | AIIMS-trained
Providing evidence-based psychiatric care
This article is for educational purposes and does not replace professional medical advice.
Common Questions About Insomnia
How many hours of sleep do adults need?
Most adults require 7–9 hours of sleep per night for optimal physical and mental functioning. Individual sleep needs may vary slightly, but consistently sleeping less than six hours can affect concentration, mood, and overall health.
What is the most common cause of insomnia?
Stress and psychological factors are among the most common triggers of insomnia. Work pressure, emotional distress, health concerns, and major life changes can activate the brain’s stress-response system, making it difficult to relax and fall asleep.
Can anxiety cause insomnia?
Yes. Anxiety can increase mental and physical arousal, making it difficult for the brain to transition into sleep. Racing thoughts, excessive worry, and heightened alertness often interfere with both falling asleep and staying asleep.
Can insomnia go away on its own?
Short-term insomnia often improves once the underlying stressor resolves. However, chronic insomnia may persist because certain behaviours—such as irregular sleep schedules or worrying about sleep—begin to maintain the problem.
What is the best treatment for chronic insomnia?
Cognitive Behavioural Therapy for Insomnia (CBT-I) is considered the first-line treatment for chronic insomnia. It helps individuals change behaviours and thought patterns that interfere with sleep and has been shown to produce long-lasting improvements.
Reviewed by Dr. Mahendra Singh Uikey
Consultant Psychiatrist | AIIMS-trained
Providing evidence-based psychiatric care
