Is Depression Really a Chemical Imbalance? What Recent Research Shows
Does low serotonin really cause depression? Learn what modern research says about the chemical imbalance theory and how depression is understood today.
DEPRESSION
Dr Mahendra Singh
5/7/20266 min read
If you’ve ever searched for information about depression, there’s a good chance you came across the phrase “chemical imbalance.”
For years, depression was commonly explained as the result of low serotonin in the brain.
The idea became especially popular during the rise of antidepressants like SSRIs in the 1990s. Over time, it moved beyond psychiatry clinics and into advertisements, internet articles, and everyday conversations.
Even today, many people still think depression has been scientifically proven to result from a serotonin deficiency.
But modern neuroscience tells a more complicated story.
A large umbrella review published in Molecular Psychiatry looked at decades of serotonin research and found no consistent evidence that depression is simply caused by low serotonin levels alone.
For many people, that finding feels confusing at first.
After all, serotonin clearly does matter in the brain. But depression itself seems to involve far more than a single brain chemical.
Sleep problems, chronic stress, emotional trauma, burnout, inflammation, genetics, and life experiences may all interact in ways that affect mood and emotional resilience over time.
So the newer research does not mean depression is “not biological.” And it definitely does not mean depression is “imaginary.”
What it suggests is something more nuanced:
Depression appears to be much more layered than the older “one chemical causes one illness” model.
Key Points
The older idea that depression is mainly caused by “low serotonin” no longer fits well with current research. Large reviews have not found consistent evidence supporting the classic chemical imbalance explanation.
Modern psychiatry increasingly views depression as something shaped by multiple interacting systems involving stress, sleep, emotional regulation, inflammation, personality, life experiences, and brain function.
Antidepressants may still help many people, but recovery often involves much more than changing one neurotransmitter.
👉 Explore more in our Depression Hub
How Did the “Chemical Imbalance” Idea Become So Popular?
The serotonin theory of depression began developing in the 1960s after researchers noticed that some medications affecting brain chemicals also seemed to affect mood.
Later, SSRIs became widely used and serotonin gradually became the centrepiece of public explanations about depression.
The message was simple and easy to understand:
| Depression happens because serotonin levels are low.
But the brain rarely works in such straightforward ways.
As research methods improved, scientists began noticing inconsistencies.
Some studies found serotonin-related differences in people with depression. Others did not. Some findings disappeared in larger studies.
Over time, researchers began moving toward broader models involving stress systems, sleep regulation, brain networks, emotional processing, inflammation, and neuroplasticity.
Gradually, depression started looking less like a single chemical problem and more like something shaped by stress, biology, sleep, personality, environment, and life experience all interacting together.
What Did the Recent Research Review Actually Find?
Researchers looked across several major areas of serotonin research — including serotonin levels in blood and spinal fluid, serotonin receptors, serotonin-related genes, and experiments designed to temporarily lower serotonin levels.
The review concluded:
| “The main areas of serotonin research provide no consistent evidence of there being an association between serotonin and depression.”
The authors also stated that current evidence does not support the idea that depression is directly caused by low serotonin activity or low serotonin concentrations alone.
None of this means serotonin is irrelevant.
It simply means the reality appears much more complicated than the neat “low serotonin causes depression” explanation many people heard growing up.
So Does Serotonin Still Matter?
Absolutely.
Serotonin remains closely linked to mood, anxiety, sleep, appetite, stress response, and emotional processing.
One reason modern psychiatry moved away from the older model is that emotions do not come from one isolated brain chemical.
The brain works through constantly interacting systems.
For example:
Chronic stress can affect sleep and emotional regulation
Poor sleep can worsen mood and concentration
Social isolation can increase stress sensitivity
Burnout can reduce motivation and pleasure
Neurotransmitters like serotonin, dopamine, norepinephrine, glutamate, and GABA all work together within these larger systems.
So serotonin may still influence depression — just not in the simplistic way it was once described.
Depression Involves More Than Mood
Part of the reason the chemical imbalance theory became so popular is that it was simple.
And honestly, simple explanations are comforting.
But depression affects much more than sadness.
People with depression may experience emotional numbness, fatigue, poor sleep, slowed thinking, hopelessness, low motivation, physical heaviness, and loss of pleasure or interest in life.
Some people mainly feel emotionally exhausted and overwhelmed.
Others describe feeling emotionally “flat.”
Some mainly struggle with anxiety, irritability, or exhaustion.
This variety of symptoms is one reason researchers now think depression likely involves multiple overlapping systems rather than one neurotransmitter alone.
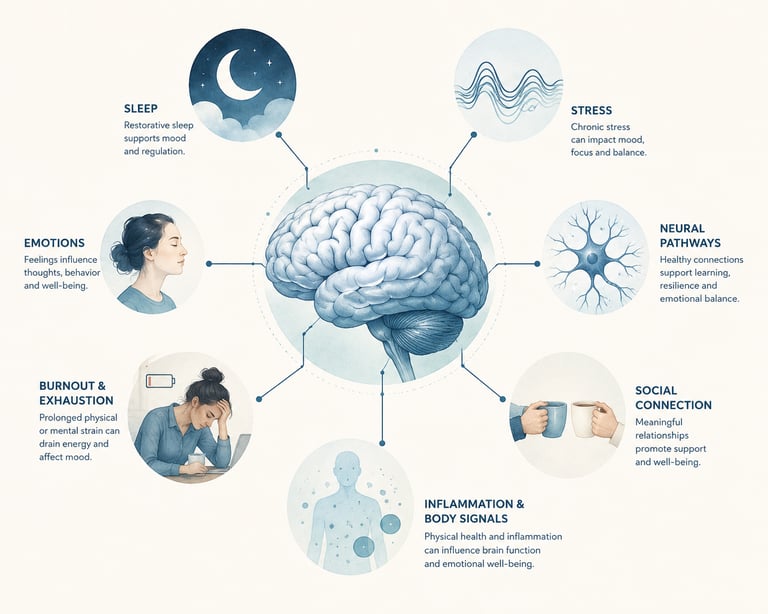
The Role of Stress, Sleep, and Burnout
Modern research increasingly highlights the relationship between depression and chronic stress.
Long-term stress can affect the body’s stress-response systems and contribute to poor sleep, emotional exhaustion, anxiety, fatigue, and difficulty concentrating.
Sleep appears especially important.
Most people who have experienced severe sleep deprivation already know this intuitively — mood, patience, motivation, and emotional control all start changing when sleep falls apart.
This is one reason sleep problems are now viewed as more than just a symptom of depression — they may also contribute to it.
Burnout, social stress, loneliness, and emotional overload may also shape how vulnerable someone becomes over time.
What About Dopamine and Motivation?
Depression is not always just about feeling sad.
For many people, the hardest part is:
lack of motivation
inability to enjoy things
emotional disconnection
feeling mentally slowed down
Researchers believe some of these symptoms may involve dopamine-related reward systems.
This again suggests that depression cannot be fully explained through serotonin alone.
What Did Genetic Studies Find?
Researchers also looked at large genetic studies involving serotonin-related genes.
Earlier smaller studies suggested there might be links between depression and certain serotonin transporter genes.
However, larger and better-designed studies did not consistently confirm those findings.
The review found no strong evidence that serotonin-related genes directly cause depression, and no convincing evidence that serotonin genes combined with stress reliably predict who develops depression.
Again, the pattern pointed toward complexity rather than a single clear cause.
Does This Mean Antidepressants Don’t Work?
No.
This is where many online discussions become misleading.
Questioning the “chemical imbalance” theory is not the same as saying antidepressants never help.
Many people do experience improvement with antidepressants.
Researchers increasingly believe antidepressants may work through more complicated effects involving emotional processing, stress sensitivity, sleep, anxiety reduction, and gradual brain adaptation over time.
And like most areas of medicine, response varies widely from person to person.
Some individuals improve significantly with medication.
Others benefit more from therapy, exercise, sleep treatment, behavioural changes, social support, or combined approaches.
Why This Discussion Matters
How people understand depression can shape how they view themselves.
Research suggests that strongly deterministic “chemical imbalance” explanations may sometimes increase pessimism about recovery or make people feel overly dependent on medication alone.
At the same time, blaming depression entirely on “mindset” can also be harmful.
The reality is probably somewhere in the middle.
Depression involves the brain, the body, life experiences, behaviour, stress, sleep, relationships, and emotional patterns — all interacting together.
That broader understanding may actually be more hopeful, because it means improvement can happen through multiple pathways.
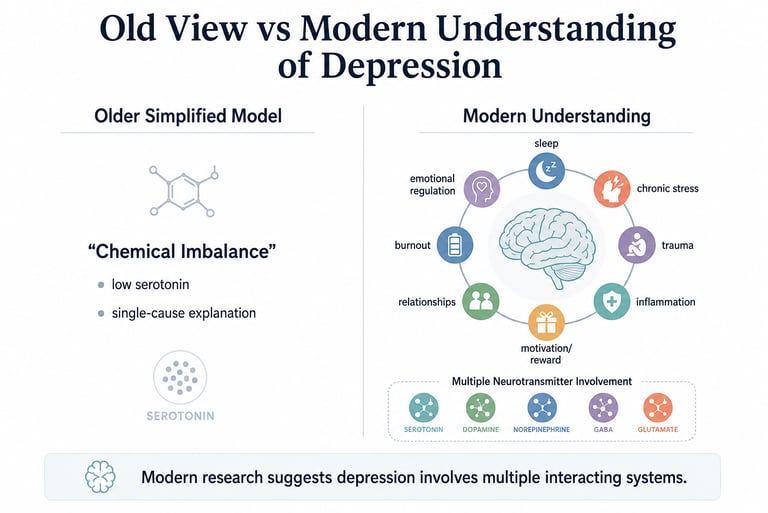
Depression Is Real — Even If It’s Not a Simple Chemical Imbalance
Depression is a real and potentially serious health condition that can affect emotions, physical energy, motivation, sleep, relationships, concentration, and daily functioning.
But most modern researchers no longer believe it can be fully explained by one neurotransmitter alone.
The brain is more complicated than that.
Human emotion was never going to fit neatly into one chemical equation.
When to Seek Professional Help
Professional support may help if symptoms such as the following persist for more than two weeks:
persistent low mood
loss of interest or pleasure
fatigue
hopelessness
sleep changes
appetite changes
difficulty functioning
suicidal thoughts
Early support can improve outcomes significantly.
Screening and Self-Assessment
Assess Depression Symptoms
👉 Take the PHQ-9 Depression Test to understand symptom severity and when professional support may help.
Assess Anxiety Symptoms
👉 Take the GAD-7 Anxiety Test to evaluate worry, restlessness, and physical symptoms of anxiety.
Assess Sleep Difficulties
👉 Take the Insomnia Severity Index (ISI) to understand whether sleep problems may be affecting mood and emotional functioning.
Frequently asked questions
Why was serotonin linked to depression?
The serotonin theory became popular after researchers noticed that medications affecting serotonin could influence mood. Over time, the explanation became widely used in public education and media because it was simple and easy to understand.
Can depression be treated without medication?
For some individuals milder severity, psychotherapy, exercise, sleep improvement, stress management, behavioural changes, and social support can significantly help. Others may benefit from medication or a combination of approaches depending on symptom severity and individual needs.
Is depression still biological if it’s not a simple chemical imbalance?
Yes. Depression clearly involves biological changes affecting the brain and body. Modern research simply suggests that these processes are more complex than a single chemical deficiency.
Reviewed by Dr. Mahendra Singh Uikey
Consultant Psychiatrist | AIIMS-trained
Providing evidence-based psychiatric care
This article is for educational purposes and does not replace professional medical advice.
